The Role of Patient Positioning in Rehabilitation
- Anuj Tiwari

- Mar 2
- 3 min read
Consider the hours spent at a desk with poor posture or resting in bed after surgery without adequate support. Over time, even seemingly simple positions can either facilitate recovery or, conversely, hinder it. The National Institutes of Health (NIH) and the American Physical Therapy Association (APTA) report that improper positioning can lead to pain, delayed healing, pressure injuries, and reduced functional outcomes.
Patient positioning goes beyond mere comfort—it is a fundamental clinical tool in rehabilitation. In this blog, you will learn how appropriate patient positioning plays a vital role in recovery by relieving pain, improving mobility, and supporting long-term functionality, as explained by a licensed clinical physiotherapist.
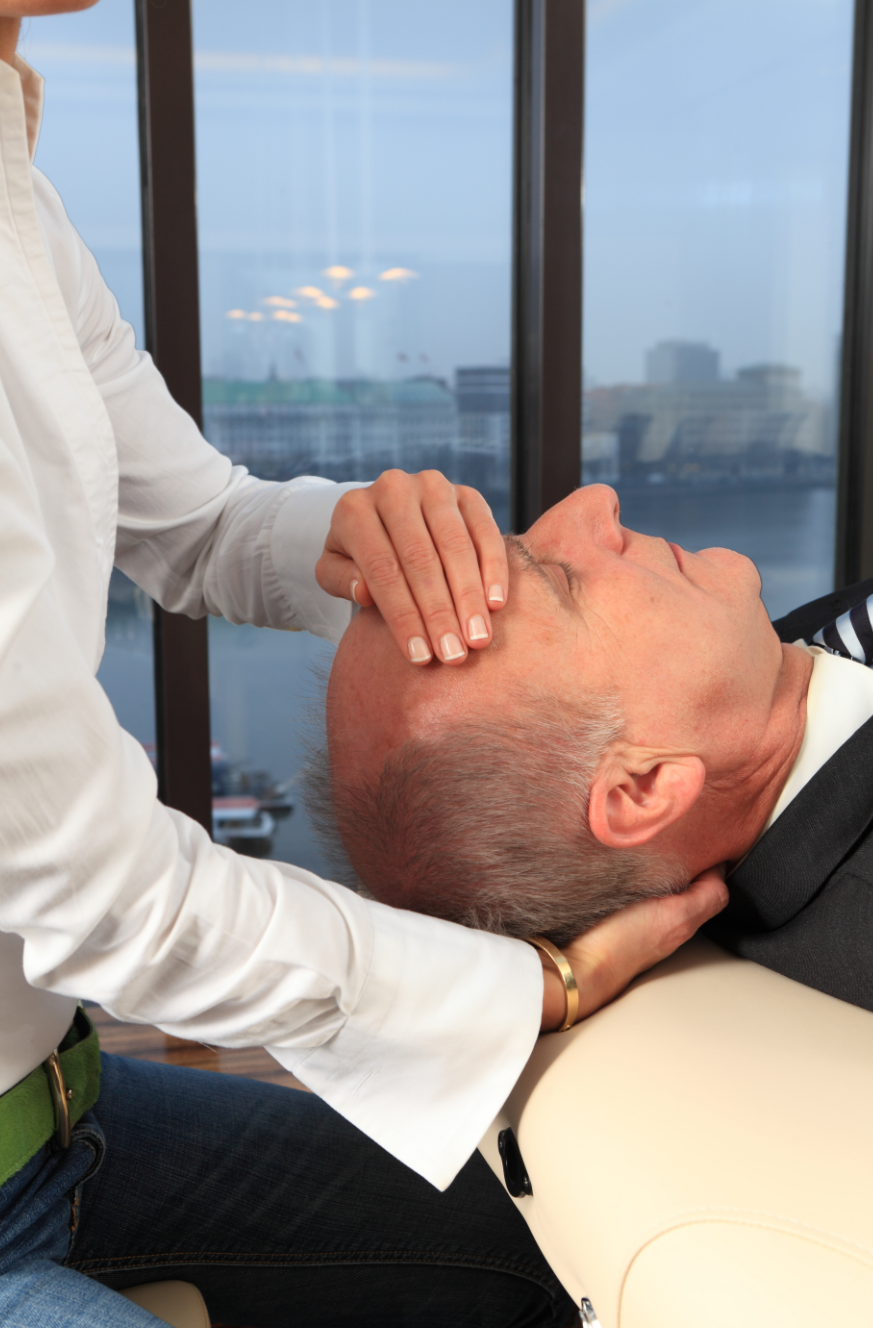
What Does Patient Positioning Mean in Rehabilitation?
Patient positioning involves intentionally arranging the body to promote healing, improve alignment, reduce stress on tissues, and maximize movement efficiency. In physiotherapy, positioning is applied during rest, exercise, transfers, and daily activities to support recovery and prevent complications
Common Reasons for Poor Positioning
Poor positioning often occurs unintentionally due to:
Prolonged desk work with a hunched posture
Improper sleeping positions
Extended driving hours
Post-surgical immobility
Lack of ergonomic awareness
Muscle weakness or imbalance
Over time, these habits place unnecessary strain on joints, muscles, and nerves.
Key Symptoms Associated with Improper Positioning
Early signs may include:
Neck or lower back stiffness
Shoulder tightness
Tingling or numbness
More severe symptoms can include:
Chronic pain
Joint degeneration
Reduced mobility
Delayed post-surgical recovery
Ignoring these symptoms can significantly affect rehabilitation outcomes.
Who Is at Risk?
Proper patient positioning is especially important for:
Office workers and remote employees
Athletes recovering from injuries
Post-operative patients
Older adults with limited mobility
Individuals with neurological conditions
Caregivers of bed-bound patients
Lifestyle habits, work demands, and physical conditioning all influence risk levels.

Impact on Daily Life
In the United States, everyday activities such as long commutes, extended screen exposure, and sedentary occupations can worsen poor positioning habits. Incorrect alignment may affect:
Work productivity
Comfort while driving
Sleep quality
Parenting and household tasks
Sports and recreational activities
Correct positioning promotes efficient movement and conserves energy.
Diagnosis and Evaluation in Physiotherapy
A physiotherapist evaluates:
Postural alignment
Muscle length and strength
Joint mobility
Movement patterns
Pain response in various positions
This assessment helps identify harmful positioning habits and guides corrective strategies.
Physiotherapy Treatment and Management
Rehabilitation programs may include:
Postural re-education
Therapeutic positioning during rest and activity
Manual therapy to reduce stiffness
Targeted strengthening and mobility exercises
Ergonomic advice for work and home environments
Proper positioning enhances the effectiveness of all physiotherapy interventions.

Home Care and Prevention Tips
Patients can support their recovery by:
Using lumbar or cervical supports while sitting
Avoiding prolonged static positions
Adjusting workstation ergonomics
Sleeping with an appropriate pillow and mattress support
Following prescribed exercise programs consistently
Consistency is key to preventing recurrence.
Real-Life Case Insight
A 42-year-old office worker in the United States reported chronic neck pain despite maintaining regular physical activity. After modifying desk posture and sleeping arrangements alongside physiotherapy treatment, pain levels reduced within three weeks, and work productivity improved noticeably. This case highlights how small positioning changes can lead to meaningful results.
When to See a Physiotherapist?
Consult a licensed physiotherapist if you experience:
Pain lasting longer than two weeks
Recurrent stiffness despite adequate rest
Post-surgical discomfort
Numbness or weakness
Difficulty maintaining proper posture
Early intervention helps prevent long-term complications.
Professional Advice from a Physiotherapist
“Patient positioning is often an underestimated yet powerful component of rehabilitation. Correct alignment promotes healing, reduces pain, and accelerates recovery when combined with individualized physiotherapy care.”
— MSK Anuj Tiwari, DivyaPhysio
Conclusion: Positioning Is the Foundation of Recovery!
Patient positioning is not a minor consideration—it is a cornerstone of effective rehabilitation. From pain relief to functional independence, proper positioning supports every stage of recovery. Seeking physiotherapy early ensures that positioning strategies are personalized, safe, and evidence-based.If pain or discomfort persists for more than two weeks, consult a licensed physiotherapist.



Comments